In this story, I’ve shared health-related details that are quite personal. I’ve decided to talk openly about this part of my health journey because I feel that there are many health issues that people are experiencing in isolation when there really is no need to. If we can talk openly about our experiences, we can not only learn more about our bodies (and therefore ourselves), but we might just feel a little less alone in our own journeys through sickness and health.
Endometriosis is estimated to affect 176 million people worldwide, and roughly 1 in 10 women in New Zealand.¹ On average it takes a person 7.5 years from the onset of symptoms to get a diagnosis of endometriosis.²
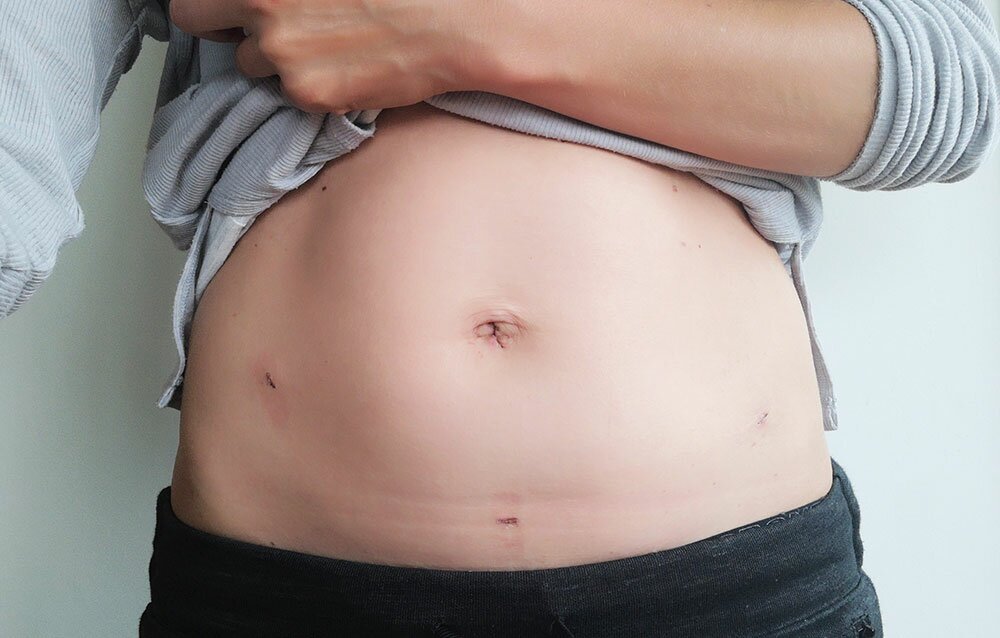
Tomorrow I will be celebrating three months since my hysterectomy. And I’m pretty sure that in the months and years to come I will look back on it as something to celebrate, which makes me very lucky indeed. Although the scars are tiny and I feel very little discomfort these days, I know I’m still in recovery – I still have frequent bouts of fatigue and headaches. However, I now feel I’m ready to write about my experience and some of the insights I’ve gained from it.
Going into this operation, I wasn’t 100% sure what was wrong with me or what the surgeon would find when she went in. Based on my main symptom of menorrhagia (heavy menstrual bleeding) which seemed to be the most obvious cause of my iron deficiency, my gynaecologist was fairly certain I had a condition called adenomyosis, and there was a chance I had endometriosis as well. Shortly before they wheeled me down to theatre, the gynaecologist came to visit me to check I was ok and to review the procedure with me. As she was talking to me I realised that I was about to entrust my body, specifically, my reproductive organs, to a person I had talked to for no more than 20 minutes in my whole life up until that point in time. I had had a total of three 5-minute appointments with her. As she turned to leave, I reached out and shook her hand. She was a little surprised, but what she didn’t realise was that it was my way of saying “I trust you” …without having to say it.
After the operation, I came to with nurses around me and we were still in theatre. The first thing I asked was, “Was there endometriosis?” and the nurse told me that indeed, I had endometriosis, and there was quite a bit of it too. Any uncertainty I felt about choosing to have a hysterectomy vanished in that instant, and I honestly haven’t looked back. I should reiterate that a hysterectomy doesn’t cure endometriosis, and I was aware of that at the time, but I guess what I felt relief about was knowing that there was something wrong with me after all. Something with a name, something that connected the dots I’ve been trying to connect for years with little success. Later on, when I met the gynaecologist for my two-week follow-up appointment, she explained that I had Stage 3 endometriosis (meaning it was advanced enough that there were adhesions from scar tissue formation) and my uterus was adenomyotic (a hysterectomy is a cure for adenomyosis). In retrospect, I consider myself to be nothing short of extremely lucky that my only serious symptoms in all these years have been the heavy bleeding and resulting iron deficiency. Instead of feeling sad that I can’t have any more children, I just feel so grateful that I have these two, and that they are healthy and happy.
But now here’s the mystery: how long have I had endometriosis for? Apparently, it takes on average 7 and a half years for a person to be diagnosed with endometriosis after the symptoms first present. I didn’t experience menorrhagia until after the birth of my first child, now six years ago. But the night before my third appointment with the gynaecologist (the one where I said, “Ok, I think I should have the hysterectomy”), I remembered something I’d forgotten till now, and I thought, “I should google this and see what comes up.” To my surprise, I discovered that painful bowel motions during your period are a classic symptom of endometriosis. When I say “painful”, I mean that I have memories of lying on the toilet floor in the foetal position, crying and seeing stars. Writing this down, I realise this sounds quite dramatic – enough to question how I could possibly have neglected to mention this to my GP or gynaecologist anytime in the last 10 years? – but there are a few reasons why I forgot about it. The first is because it only happened one, or maybe two days a month. The second is because as soon as I had passed a motion I was perfectly fine again. The third is because I did mention it to a couple of people and I didn’t get the sort of response from either to make me feel like I should rush to the doctor and get some answers. One of them was my husband, and I recall he truly didn’t know what to do with the information – he probably said something very sympathetic and gave me a cuddle. The other person was my mum, and I can’t now recall her exact response when I told her I’d just picked myself up off the bathroom floor, but knowing her it would have been something along the lines of “What? That’s weird… Huh. (…and change of topic.)” My mum isn’t heartless or unsympathetic; she just belongs to a different generation from me. A generation of mums who lived with these problems themselves and figure, well, it didn’t kill them and they got through life all right, so I’m sure you’ll figure out a way to get through it. Or perhaps it’s not a generational thing. My mum didn’t have a mum, so she just had to work through these difficulties on her own, and she did. (Now I know that endometriosis is hereditary, there’s a very good chance my mum has lived with endometriosis her whole adult life with no diagnosis.) The last (but probably most significant) reason is that I’m pretty sure I haven’t experienced this crippling pain for about a year, maybe two. The last time I recall being in such pain was when we were still living in our old house, the one we sold in July 2017. And I have a hunch as to why that might be, which I am very keen to share with you!
The Mrs Goodness blog was born way back in March 2016. I intended to record my new journey into ‘good’ living, and hoped that other people reading it might find something useful or inspiring for themselves. Over the past 3 years I’ve shared how I have cleaned up my diet and my home, in part to make my life more environmentally sustainable, but mostly to make my life sustainable for me. I’ve been on a personal mission to create a lifestyle for myself that promotes good health and wellbeing, and many of the changes have been dietary. In trying to naturally manage menorrhagia, low iron, (embarrassingly) excessive flatulence and bloating, I have chosen to quit dairy, gluten, refined sugar, caffeine, and processed foods in general, replacing them with whole foods, as many vegetables as possible, and fermented foods. I felt sure I was making progress with every incremental change, and that I was just one step away from figuring out the root cause of my symptoms. But late last year, when I learned my iron stores were at rock-bottom levels despite my fantastic diet and all these lifestyle changes, I have to confess I felt defeated. To be told I had adenomyosis, a condition I’d never heard of before, when I’d been so sure I had some sort of gut dysbiosis (SIBO? gluten intolerance? fructose malabsorption?) was totally deflating, and very humbling too I might add. But then I did some basic research into the diseases of adenomyosis and endometriosis, and I learned that while their causes are not yet known, both are inflammatory diseases. Which means that their progression (and the amount of pain associated with the disease) would be exacerbated by stress and a pro-inflammatory diet. – 🙋 Wait, what’s a pro-inflammatory diet? It’s a diet rich in foods that promote inflammation, such as sugar, refined vegetable oils, red and processed meats, refined grains, artificial food additives like MSG, and dairy for people who are sensitive or intolerant to it. Basically, all the things I’ve been systematically cutting out of my diet for the past few years, and replacing with (inflammation-reducing) whole, real, and fermented foods! I am quite certain that my pain and discomfort have been reduced significantly thanks to the transformation of my diet. Since realising this, instead of feeling defeated, I now feel proud of myself – and lucky. You see, I believe that for the past few years I’ve been inadvertently managing a disease I didn’t know I had! Even if I had known that I had endometriosis and adenomyosis for all these years, I feel pretty sure I would have done exactly what I’ve done anyway. And who knows, perhaps instead of doing it from an empowered perspective, as I have done, I might have done it all feeling more like a victim, feeling like I was forced to make these changes because of the disease…
The hysterectomy hasn’t been a quick and complete guarantee for perfect health. I’ve been experiencing a lot of headaches lately, and I still have menstrual cycles which I’m trying to figure out (I kept my ovaries). I have mild-moderate pelvic organ prolapses (from childbirth) which I need to be proactive about managing to keep them from getting worse. I will still have to work on balancing my hormones as I recover and then begin to head towards menopause. But something amazing has come from this operation that was quite unexpected! Ever since the operation, my digestion has been NORMAL. No excessive farting (I still fart, but only like a normal person, haha 😳), no belly aches from wind. I can eat fruit! And onions and garlic! And I can enjoy them too, without fearing the consequences. Never in a thousand years did I expect that my digestive discomfort was due to problems with my reproductive organs, but it turns out that endometriosis symptoms are commonly mistaken for digestive disorders such as IBS³ because the symptoms can be so similar. Over the past year, I’ve had more than one well-meaning friend/family member suggest that perhaps my food sensitivities were psychosomatic? That perhaps I was obsessing over food so much that I was making things worse? These comments were made from genuinely caring, sincere points of view, and so when I couldn’t get complete relief, no matter what I ate or didn’t eat, or how much I researched, I really did start to wonder if they were right. Was I my own problem?
As you can imagine, this unexpected outcome has left me feeling soooo vindicated. Although I couldn’t work out what was wrong, I knew something was wrong, and I was right. It took a long time, but I trusted myself, I listened to my body, and I listened to the advice of others. Now I have some answers, but instead of feeling defeated and deflated, I feel like I own my own body, I own my health, and although I needed medical intervention to get me here, I know I’m not powerless; every day I have the means to support and nurture my body towards good health through my dietary and lifestyle choices.
PS. My ferritin levels are now almost optimal – my last blood test a few weeks ago indicated I have a ferritin level of 68μg/L! My ferritin level has steadily climbed since I had the iron injections and stopped menstruating. I feel more confident now about removing red meat from my diet, something I have been interested in doing for a while (for various reasons) but felt I couldn’t do when I knew I had iron deficiency.
¹ https://nzendo.org.nz/endo-information/
² https://thefemedic.com/menstruation/why-take-long-diagnose-endometriosis/
³ Although it would seem that endometriosis and IBS are linked so perhaps it’s less about ‘misdiagnosed’ and more about ‘incompletely diagnosed’? https://badgut.org/information-centre/a-z-digestive-topics/endometriosis-and-ibs/
Hi Esther, read your post.
Never knew you had all these problems but at least you worked out a solution for you and a management program that helps you.
Endometriosis is not funny and a real problem for many, especially if it is not diagnosed.
Keep going girl you are a fantastic person, I was only a gut nurse for 50 years, but was never asked or knew about your problems. Life teaches us lessons when it comes to our own bodies that nobody can predict.
Good on you, big hugs Agnes xxx